Osteoarthritis Self-Test
Osteoarthritis is a degenerative joint disease that can begin to develop early in life. However, changes in the articular cartilage are usually only discovered once pain is obvious. Since it may take years or even decades after the initial cartilage injury, we advise everyone to perform an osteoarthritis self-test.
Rarely do people remember accidents and injuries that occur when they are younger. This means that they don’t realize that they are at risk of developing osteoarthritis later in life. Unfortunately by the time pain and joint problems are apparent, the joints are already at a stage of advanced destruction.
However, if arthritis is discovered earlier then patients can have greater control over their future joint health.
Are there absolutely methods to detect osteoarthritis before it causes problems? What tests can help the patient?
Imaging techniques and joint arthroscopy for suspected osteoarthritis
During a medical examination doctors will discuss the patient’s medical history and perform functional tests. This can help to assess the risk of developing joint diseases such as osteoarthritis.
However, this alone is not sufficient to make a definitive diagnosis. Imaging techniques are used to further examine joint health1.
X-rays of the joint
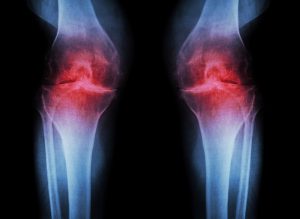
X-rays remain a popular means to assess bone structure. However, cartilage and soft tissue remain invisible. An x-ray will reveal any narrowing of the joint space or bone deformities in advanced osteoarthritis.
Unfortunately, early damage to the cartilage cannot be determined using x-rays2. Specialists point out that the joint space in the X-ray can be measured correctly only under load. In other words: the radiograph should always be preformed standing to determine the correct joint space of the knee, foot, or hip joints.
Magnetic Resonance Imaging
Other imaging methods include magnetic resonance imaging (MRI) and ultrasound (sonography). The advantage of these methods is that they do not release any radiation and the soft tissues and cartilage can be easily seen. Inflammation and synovial fluid can analysed using these methods, although it’s difficult to distinguish between different types of arthritis.
Arthroscopy
The most decisive way to determine the possible onset of osteoarthritis is an arthroscopy. This is a minor surgical procedure. It involves a small incision made at the joint and a camera inserted to assess the condition of the joint. The synovial fluid can then be tested for inflammatory markers and autoantibodies. The results can help to determine if the patent is suffering from osteoarthritis or arthritis.
Arthroscopy also offers the advantage of performing joint-preserving measures during the procedure. For example, the cartilage surfaces can be smoothed over and bone fragments may be removed. However, this methodology is not without controversy, as it exposes the joint to the risk of infection3,4,5.
Self-tests and their expressive possibilities
We have developed a short questionnaire so that you can perform a self-test at home to assess your risk of osteoarthritis. The test involves just a few clicks. It is completely anonymous and free. Based on the result, you will have an indication on how to interpret your joint pain.
Please note*
In every case, this test cannot provide a diagnosis. A doctor must be consulted for joint problems. This osteoarthritis self-test is a reliable means to determine the personal risk of developing osteoarthritis. It takes takes into consideration all the key variables leading to a personal risk factor, including physical activity, diet, and age.
However, this osteoarthritis self-test doesn’t provide definitive diagnosis about whether someone is suffering from osteoarthritis or other inflammatory joint disease. Only the propensity to develop such a disease is assessed in this test. This test can help the person seeking advice to reassess their lifestyles and make positive choices that will help to reduce the risk of osteoarthritis (diet, joint-gentle sport, exercise, dietary supplements, avoiding obesity).
References
- “Sankowski, A. et al. (2013). Psoriatic Arthritis. Polish Journal of Radiology. Volume 78, Issue 1, (pp. 7-17).” ↩
- “Sutter, R. et. al. (2012). New developments in hip imaging. Radiology. Volume 264 , Issue 3, (pp. 651-67).” ↩
- “Elfeddali, R. et al. (2013). Arthroscopic elbow surgery, is it safe? Journal of Shoulder and Elbow Surgery. Volume 22, Issue 5, (pp. 647-52).” ↩
- “Bert, J. and Bert, T. (2013). Management of infections after arthroscopy. Sport Medicine & Arthroscopy Review. Volume 21, Issue 2, (pp.75-9).” ↩
- “Noud, P. and Esch, J. (2013). Complications of arthroscopic shoulder surgery. Sport Medicine & Arthroscopy Review. Volume 21, Issue 2, (pp.89-96).” ↩






