Knee Arthroscopy – Investigating Joint Preservation
 Advanced stages of knee osteoarthritis (coxarthrosis) will lead to the complete destruction of the articular cartilage. This is accompanied by serve inflammation and pain. This can be very debilitating as mobility is significantly reduced. Managing the pain using pain-killers is not a long-term option due to the potential health risks. Consequently, a knee arthroscopy is often necessary. Knee replacement surgery is often considered as a last resort, with joint preservation measures firstly investigated.
Advanced stages of knee osteoarthritis (coxarthrosis) will lead to the complete destruction of the articular cartilage. This is accompanied by serve inflammation and pain. This can be very debilitating as mobility is significantly reduced. Managing the pain using pain-killers is not a long-term option due to the potential health risks. Consequently, a knee arthroscopy is often necessary. Knee replacement surgery is often considered as a last resort, with joint preservation measures firstly investigated.
If osteoarthritis isn’t fully developed, a knee arthroscopy can be applied. This is a minimally invasive procedure. Using small incisions, the knee joint is investigated using a probe. The synovial fluid is flushed to remove any fragments of cartilage and bone that have accumulated over the years. Minor surgery may also be performed during the procedure to minimize joint abrasion. A knee arthroscopy can help to restore movement and minimize joint pain.
However, there’s a general consensus that knee arthroscopy rarely actually prevents the development of osteoarthritis. The pain relief is only temporary and patients need to continue to support healthy joint maintenance. Many physicians encourage patients to participate in low impact exercises, such as walking, swimming and cycling. This helps to stimulate the lubricating synovial fluid and relives the joints. The leg muscles are also strengthened to better support the knee joint.
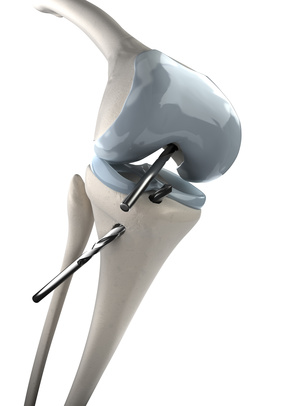
Knee Prosthesis – The Last Resort
For some patients, having knee replacement surgery is the only option. One of the problems that many patients experience following this surgery is that their expectations aren’t fulfilled in terms of mobility and pain relief.
There is no single artificial joint that can replace the natural knee in its movement and strength. Most people are able to achieve around three-quarters of total knee movement capacity. Activities such as kneeling can be painful due to placing weight on scar tissue. There are often clicking and clunking sounds associated with moving the artificial knee. Also, the replacement joint will wear out over time and may become loose.
Usually knee replacements will last for around 20 years. Repeat knee operations may be necessary for individuals that are overweight, involved in heavy manual labor, or play vigorous sport. Repeat surgeries become more complicated and the benefits decline with each revision.
Older people tend to have more difficulties with knee replacement surgery. Japanese researchers found that older people often have much less blood. This is because they tend to drink less and this decreases their blood volume. Since the entire knee requires replacement with a metallic implant, knee surgery is associated with a very high loss of blood. Researchers recommend that in order to meet the demand for blood during the procedure, patients should perform autologous blood donation before major surgery with a haematocrit less than 11g/dl1.
Doctors Assess Treatment Success Differently Than Patients
In 2011, U.S. researchers found that the self-assessment of surgical patients greatly differed from the opinion of their doctors2. One hundred and forty patients were asked about their feelings of pain and mobility after knee surgery.
Over a period of weeks after their self-assessment, a physician assessed the individual patient. During the evaluation it was noted that the doctor rated the success of the procedure more positively than the patient. Patient pain and functionality scores recorded were much worse than the doctor-assessed scores.
However, whether the artificial knee improves mobility is also a matter of personal fitness and lifestyle. Staying fit and maintaining a healthy body weight are very important if knee surgery is to be successful.
Bibliography:
- Fujimoto et al. 2003. “Blood loss in patients for total knee arthroplasty.” Knee Surg Sports Traumatol Arthrosc. 11(3): 149-54). ↩
- Khanna et al. 2011. “Comparison of patient-reported outcomes and clinician-Assessed Following Following total knee arthroplasty.” J Bone Joint Surg Am. 93(20): e117(1)-(7). ↩






